Gum Disease Treatment
in Seal Beach
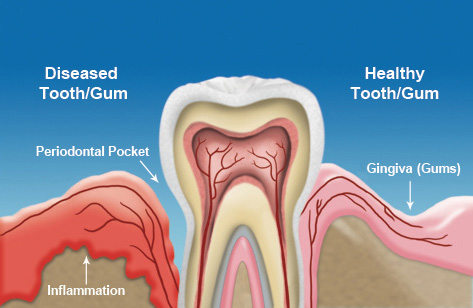
Gum disease, also known as periodontal disease, is the most common cause of tooth loss in adults. As the disease progresses, it causes increasing damage to bone and gum tissue, which causes teeth to loosen and eventually fall out. Because of his specialty training and experience, Dr. Aslam is often able to save teeth that otherwise might have been lost to the disease.
Dr. Aslam has a variety of procedures at his disposal for treating your mild to severe periodontal disease and reversing its negative effects. These include periodontal deep cleaning, supplemental antibiotic therapy and surgical methods.
Call 562-262-5595 or click here to schedule an appointment.

Skilled Gum Disease Treatment Specialist
As a board-certified periodontist, Dr. Aslam has extensive advanced training in diagnosing and treating all stages of gum disease, as well as repairing the damage it causes. When needed, Dr. Aslam uses advanced gum and bone grafting techniques to rebuild tissue that has been lost to the disease, providing a stable foundation for saving teeth.
Who Should See a Periodontist for Gum Disease Treatment?
Anyone can benefit from seeing a periodontist for gum disease treatment, but patients who are smokers or diabetics can especially benefit from Dr. Aslam’s advanced periodontal expertise. These latter types of gum disease cases are frequently more complicated and require an expert periodontist to correctly and effectively treat them.
Call 562-262-5595 or click here to schedule an appointment.
